 
These findings suggest that OCT could have excellent diagnostic potential in the ED, at minimum as a highly sensitive screening test for RD. Both imaging modalities had high specificities with no significant difference. 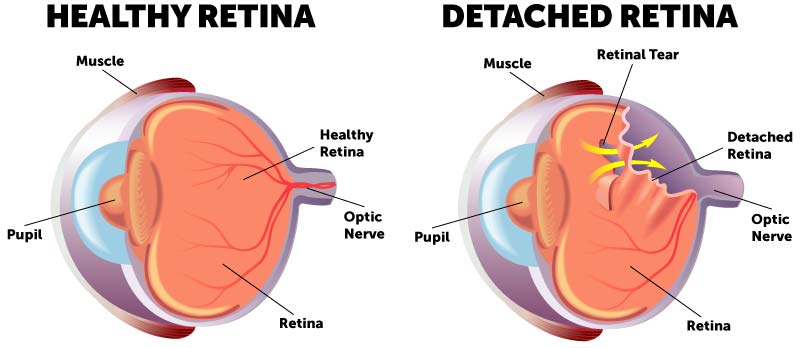
There was no significant difference in specificities between OCT and fundus photos (z = 4, p = 0.7500).ĮD clinicians detected RD with greater sensitivity on OCT images than on fundus photos. WSRT indicated that sensitivity on OCT was statistically significantly higher than sensitivity on fundus photos (z = 0, p = 0.0039). Wilcoxon signed-rank test (WSRT) was used to compare the paired differences between fundus photos and OCT images.ĮD clinicians achieved 97% sensitivity and 93% specificity on OCT images as compared to 75% sensitivity and 96% specificity on fundus photos (Table 1). Sensitivity and specificity were calculated for each imaging modality using the retina specialists’ prior interpretations as the gold standard. Each clinician first reviewed a handout on the detection of RD on fundus photos and OCT images, and then evaluated all 110 images for the presence of RD. Nine ED clinicians at Duke Health participated in this study. All images were acquired and interpreted by retina specialists as part of routine clinical care. One fundus photo and one paired OCT image were used from each eye for a total of 110 images (Figure 1). This study tested the hypothesis that ED clinicians can detect RD with greater sensitivity and specificity on OCT images versus en face fundus photographs.Ī retrospective dataset was assembled from 55 eyes (30 with RD, 25 without RD) recently treated at Duke Eye Center. Optical coherence tomography (OCT) is a promising alternative that offers cross-sectional images of the retina with micrometer resolution. Current standard of care in the emergency department (ED) is to examine the fundus with a direct ophthalmoscope, a difficult-to-use instrument with a limited en face view. It is important to report any new visual symptoms of floaters, flashes, or peripheral shadows to an eye care professional immediately to increase your chances of preserving vision.Retinal detachment (RD) is an ocular emergency that can quickly progress to complete loss of vision without prompt diagnosis and treatment. Detached Retina: Pneumatic Retinopexy Video.There are three main treatment options for retinal detachment and sometimes a combination of approaches is utilized depending on the characteristics of the detachment. Unfortunately, most retinal detachments require surgical intervention. If tears are detected prior to development of a retinal detachment, they may be treated with laser to prevent the detachment from occurring. The vitreous separation can tear the retina and allow fluid to pass underneath the retina, thereby detaching it from the back wall. Most retinal detachments are caused by the separation of the vitreous gel which fills the core of the eye and naturally separates between the ages of 50-70. These include nearsightedness (myopia), previous eye surgery such as cataract surgery, history of eye trauma, retinal detachment in the fellow eye or in a family member. There are several conditions that increase the risk of developing a retinal detachment. In some cases, patients may not have any symptoms until there is significant progression of the detachment. 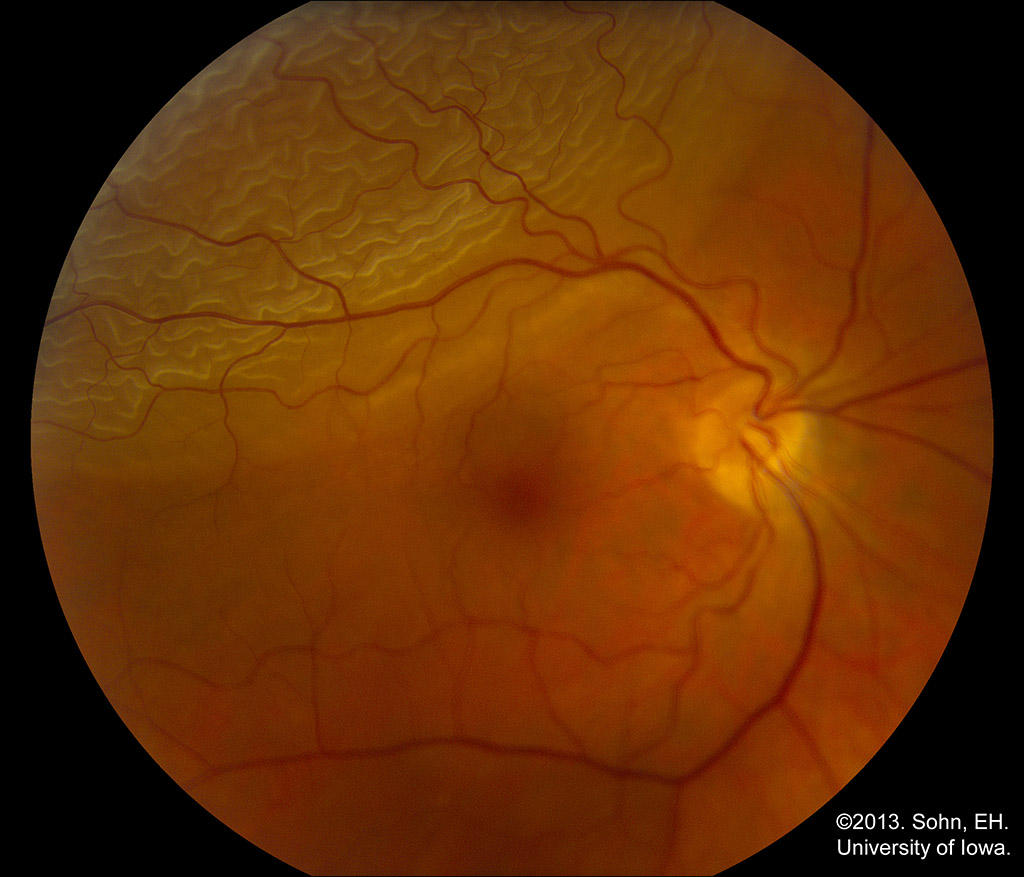
The typical symptoms of a retina detachment include sudden onset of new floaters, flashing lights, and a shadow or curtain in the peripheral vision. By Nichole Lewis from Retina Image Bank, 2017 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
